Variations in the Severity of COVID-19
In this post, I will cover some of the hypotheses of why COVID-19 is more severe for some people than others. Much of this information comes from clinical observations of COVID-19 patients that are correlated with poor disease outcomes, and scientists and physicians and hypothesize that these could be linked to disease progression.
Age, Comorbidities, and Being Male Increase COVID-19 Severity
A big question surrounding COVID-19 is why some people infected with SARS-CoV-2 get more severe symptoms than others. There is no preexisting immunity in humans against SARS-CoV-2 because no virus that is very similar to it has broadly infected the population. The SARS and MERS outbreaks infected fewer than 10,000 people each, so there was no herd immunity in the population, and the true number of people who have had recent colds caused by the mild coronaviruses (called HCoV-229E, -NL63, -OC43, and -HKU1) is unknown.
People who are older are at greater risk of severe COVID-19 and death due to preexisting chronic health conditions (comorbidities). SARS-CoV-2 primarily affects the respiratory tract and the ability of the blood to carry oxygen, and many of the common chronic conditions in developed countries, such as diabetes, hypertension, asthma, chronic obstructive pulmonary disease (COPD), obesity, and cardiovascular disease, all affect the cardiovascular and respiratory systems. These conditions don’t necessarily make it easier for SARS-CoV-2 to infect cells, but they increase the severity of COVID-19 and risk of death by making it more difficult for patients to recover.
Differences between people’s immune systems may be the reason for different disease outcomes, but this encompasses many factors. Aging of the immune system makes it slow to respond to future infections. The adaptive immune system is more so affected, making it difficult for older adults to retain immunity to an infection after they recover (side note: this is something to consider when developing vaccines because they may not work as well in the elderly). As people age, fewer and less diverse T cells (T lymphocytes), which are responsible for many functions in adaptive immunity, are produced because of shrinking of the thymus (a small organ in the chest), where T cells mature 1,2.
Based on data of around 72,000 COVID-19 cases (including asymptomatic ones) in Wuhan, China through mid-February 2020, the case fatality rate (deaths per number of diseases) and the infection fatality rate (deaths per number of infections, including asymptomatic ones) are higher for men than for women 3,4. In Italy, Spain, and New York City, men are more likely to be in the intensive care unit (ICU) and die from COVID-19 5, but there is a severe lack of data in the United States on demographics of COVID-19 infections and deaths. However, data from previous SARS and MERS outbreaks suggests that men are more likely to have severe disease and poor outcomes 6,7. The discrepancy between men and women may be due to immunological differences.
Female humans have two X chromosomes, while males have only one. The X chromosome contains the largest number of immune-related genes of any of the chromosomes 8. In each cell of a female, one of the two X chromosomes is inactivated, and the inactivated one is different in each cell, 9 as shown below.
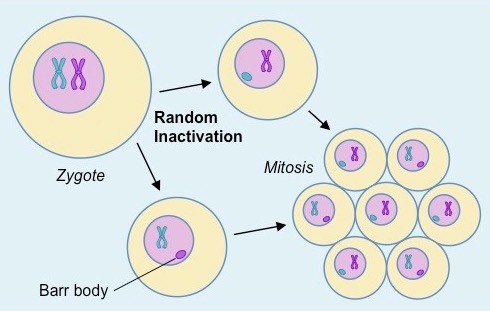
The inactivated X chromosome is called a Barr body, and when cells replicate through mitosis, each new cell undergoes random inactivation. So females don’t make double the amount of protein from the X chromosome, but they may have a greater variety because they can make proteins from both X chromosomes.
Women produce more antibodies in response to infection, vaccination, and trauma, while men exhibit more severe inflammation 10. In addition, more than three quarters of the 20 million Americans with autoimmune diseases are women, suggesting that the immune systems of women tend to be more robust than those of men, but they can, in fact, be too strong 10. A stronger immune system could be an evolutionary advantage for women during pregnancy to allow them to tolerate the developing fetus (half of the fetus’ antigens come from the father, so they are foreign to the mother’s immune system). This could make women better at clearing SARS-CoV-2 and other pathogens early before diseases worsen. There is also some evidence that approximately 5-10% of X chromosome genes may escape inactivation, possibly bolstering the immune system 11.
An interesting point is that the gene for ACE2, the receptor used by SARS-CoV-2 to bind to host cells, is found on the X chromosome. Although this could be a potential cause for different case fatality rates between men and women, a study of common genetic polymorphisms, or forms, of ACE2 in SARS patients showed that even though men had a higher mortality rate 12, the difference is not due to differences in ACE2 13. Since SARS-CoV and SARS-CoV-2 both use ACE2 to attach to cells, it is reasonable to assume that ACE2 polymorphisms would not affect disease outcomes for COVID-19 either.
Variations in Immune Cells and Antibody Types
Severe COVID-19 and death have also been correlated with a high neutrophil to lymphocyte ratio (NLR) 14. Neutrophils are part of the innate immune system, and they rapidly appear at infection sites to engulf pathogens and promote inflammation 15,16. High NLR is associated with increased likelihood of death from severe inflammation (COVID-19 appears to manifest this way) and low activity of natural killer (NK) cells and T cells 17. NK and T cells are lymphocytes that kill infected host cells, and they secrete IFN-γ, a cytokine that inhibits viral replication and increases further lymphocyte activation 18,19. A high NLR results in a weaker adaptive immune response and fewer memory B and T cells, which protect against reinfection by the same virus. Excessive inflammation caused by neutrophils can also inhibit memory B cell proliferation.
Among 61 COVID-19 patients in Beijing, China in January 2020, those with moderate/severe disease had a higher NLR and more bacterial infections than patients with mild symptoms 20. Patients with severe COVID-19 symptoms in Wuhan in January and February 2020 had more cytokines and fewer T cells in the blood 21, and T cells were the most severely reduced group of lymphocytes 22. The diagram below shows how cytotoxic T cells (which have CD8 receptors) are necessary to clear viral infections by killing infected cells.
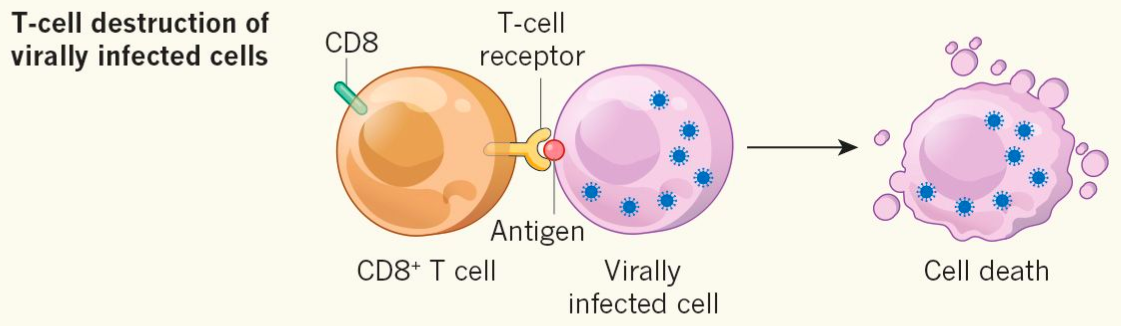
Immunoglobulin A (IgA) is another class of antibodies found primarily in mucous membranes. Mucous membranes, which contain specialized epithelial cells, protect against dehydration and pathogens, and IgAs are primarily found in respiratory and gastrointestinal secretions, such as tears, saliva, and mucus (only ~10% circulate in the blood). IgAs are important for neutralizing viruses and preventing them from infecting epithelial cells, but they also neutralize bacterial toxins. Many people with selective IgA deficiency are asymptomatic because their bodies still produce other types of protective antibodies, but some tend to have higher incidence of infectious diseases (primarily respiratory and gastrointestinal), allergies, asthma, and autoimmune diseases 23,24,25. Robust IgA activity may contribute to mild COVID-19 cases because SARS-CoV-2 could be cleared early before it gets to epithelial cells in the lower respiratory tract. This is all speculation and would be an interesting topic to research.
SARS-CoV-2 in the Young
Young people make up a smaller percentage of COVID-19 deaths, and this has been the case in all countries hit hard by SARS-CoV-2. Children have lower mortality rates, less severe disease, and require less hospitalization 26. A large reason for this is that young people have fewer comorbidities, and their innate immune systems tend to respond faster to infections than those of older people.
There is some speculation that children may have different ACE2 expression than adults, but this is unlikely to be the cause of more severe outcomes in older adults because SARS had a 0% mortality rate in people under the age of 24 and a mortality rate higher than 50% for people aged 65 and older 27. SARS-CoV and SARS-CoV-2 both use ACE2 to enter cells, so if ACE2 expression was the reason for different COVID-19 outcomes, we would not already have seen COVID-19 deaths in children, adolescents, and younger adults.
Another hypothesis is that children get more colds, on average, and some of these colds are caused by mild coronaviruses. This may provide them with some protection if their immune systems react to sequences that are similar across many coronaviruses, including SARS-CoV-2. Children may get milder forms of COVID-19 if they have cross-reactive antibodies, which react to similar but not identical epitopes on multiple coronaviruses.
A very interesting possibility is that some childhood vaccines may induce innate immunity to other viruses, including SARS-CoV-2. Live-attenuated vaccines may especially stimulate the innate immune system because they simulate virus infection and replication in cells, but the virus is too weak to cause disease in humans. These vaccines could temporarily boost the immune system, even against viruses that are completely different from the virus in the vaccine. Children may have more residual non-specific immunity because they recently received vaccines like measles, mumps, and rubella (MMR) and varicella (chickenpox). Some countries with high tuberculosis incidence still vaccinate against it; this live-attenuated vaccine is called Bacille Calmette-Guérin (BCG), and it may similarly stimulate the immune system, even though tuberculosis is caused by a bacterium.
Some scientists are calling for clinical trials to study the efficacy of such vaccines to provide short-term protection against SARS-CoV-2. They are especially interested in Albert Sabin’s oral polio vaccine (OPV) because there was evidence that it protected people in the Soviet Union against influenza in the late 20th century 28,29,30. These vaccines will NOT provide long-term adaptive immunity against SARS-CoV-2, only a short-term boost to the immune system for broad protection. But repurposed live-attenuated vaccines could be a way to slow the number of new COVID-19 infections and deaths until we can make a SARS-CoV-2 vaccine.
Conclusion
The differences we’ve seen in how COVID-19 patients fare is most likely due to different immune responses to SARS-CoV-2. Some trends, like old vs. young, are broadly applicable because weaker immune systems and more comorbidities make it more difficult for people to recover from many viral and bacterial infections. But COVID-19 can be deadly even in young, healthy people because it causes severe pneumonia and life-threatening damage to the lungs and other organs. We don't yet know why some seemingly healthy people develop life-threatening symptoms, but the answers could also help us understand other diseases.
Leave a Comment